Focused echocardiography in the emergency department, also known as cardiac ultrasound, is a valuable tool used to help diagnose and manage a diverse array of cardiovascular pathology. In this post, we will be going over the basic techniques and indications; future posts about pathology will follow. If you are a novice ultrasonographer, pay attention. If you consider yourself a pro, a little review never hurt.
Indications:
- Chest pain
- Dyspnea (Your patient has CHF and COPD? Oh no, which one is it? Use the ultrasound and find out!)
- Cardiac Arrest (Does your patient still have cardiac activity?)
- Congestive Heart Failure
- Cardiac Tamponade
- Pulmonary Embolism
- Hypotension
Equipment:
- Ultrasound machine
- Phased Array AKA “Cardiac Probe.”
- Ultrasound gel
- Patient
- Your hand
Focused Bedside Echocardiography:
- Subxiphoid view
- Para-sternal long axis view
- Para-sternal short axis view
- Apical 4 chamber view
Positioning:
Ideal Position: Left Lateral Decubitus position with left arm raised above head. This position approximates heart towards chest wall and spreads the ribs.
A male patient requires an exposed thorax. For female patients, be sure to cover up areas not being examined in order to minimize exposure of breasts.
A patient in respiratory distress might need to be scanned in upright sitting position or supine, while those with hemodynamic instability may have to be scanned in supine position. (Note: echocardiography should not come before stabilization of a hemodynamically unstable patient. It should be done afterward or better, concurrently.)
Technique:
The phased array probe is used for all views. Remember to clean/decontaminate the probe prior to placing on a new patient.

Make note of the direction of the probe marker in all views. In our probe it is denoted by the raised circle at the top.
Use the phased array probe; alternatively, the convex probe can be used in this position, such as used in the FAST exam.
- Grab the probe with both the volar and dorsal aspect of your hand above the probe, making sure your hand and finger are not touching the patient’s chest.
- Place the probe in the subxiphoid area, located in the epigastrum just below the xiphoid, at the apex of the costal angle
- Flatten the angle of probe and point towards the chest, so that it is nearly parallel to the skin.
- Ultrasound waves travel better through water than solids. Use the highly vascular (watery) liver as an acoustic window by pointing the probe initially more to the right. With the probe angle still flattened and using the liver as an acoustic window, slowly start pointing the probe more to the left.
- Increase or decrease the depth accordingly depending on your patient’s habitus.

Subxiphoid view. Arrow denotes the direction of the probe marker

Subxiphoid view. Arrow denotes the direction of the probe marker

Parasternal Long Axis view (PLAX):
- Place the probe on the left parasternal side of the chest, at about the 4th or 5th intercostal space.
- Point the probe marker towards the patient’s right shoulder.

PLAX view. Probe marker pointed to right shoulder. Note patient placed in left-lateral decubitus position

If patient unable to tolerate left-lateral decubitus, place supine. Probe marker still points to right shoulder

PLAX AO: Aorta AV: Atrial Valve DA: Descending Aorta LV: Left Ventricle MV: Mitral Valve RV: Right Ventricle
Para-sternal Sternal Short Axis (PSSA):
- In the same position as the PLAX, turn the probe’s marker counterclockwise 90 degrees to the patient’s right hip.
You can fan up or down in the PSSA view to get different levels of views: aortic valve, mitral valve, papillary muscles, and the apex.

PSSA with probe marker pointing to right hip. Left-lateral decubitus position

PSSA in supine position if unable to tolerate left-lateral decubitus, probe marker to right hip

PSSA view of the aortic valve

Level of the Mitral Valve


If assessing global LV function, use the view at papillary muscle level.

PSSA at level of the papillary muscles
Apical 4 Chamber view:
- Ideally patient is in left lateral decubitus position. If supine, have patient lift her or his arm over their head to separate their ribs.
- Find the Point of Maximal Impulse (PMI) through palpation on the left side of the chest. Place your probe in this area.
- Point your probe marker towards the patient’s right hip with the probe in the PMI on a coronal plane. Also, be aware that the PMI might not be at level of nipple in those with cardiomegaly

Palpate for PMI first

Apical 4. Left lateral decubitus. PMI near the nipple, probe marker to R hip

Apical 4 supine. PMI near the nipple in this patient. Probe towards right hip
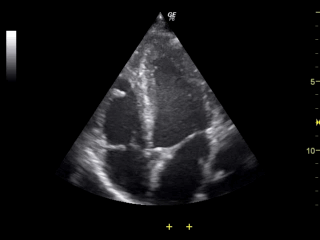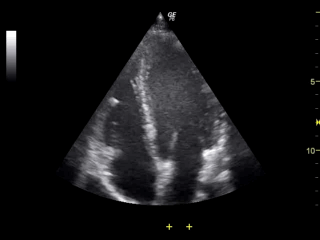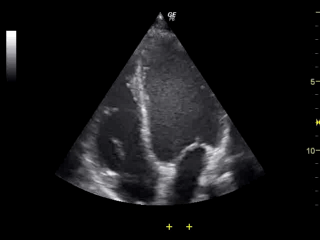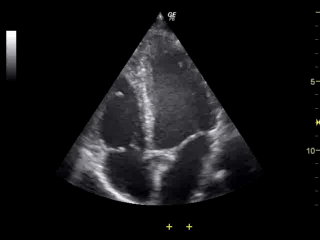
Note the LV on the right side of the screen, appearing as the largest chamber.

Apical 4 chamber view
Cardiac ultrasonography is now considered to be one of the main-stay tools in the ED. From its infancy in the ED, cardiac sono has proven to be effective. It can detect pericardial effusion in a quick and reliable manner (1) in penetrating cardiac injuries leading to faster times to the operating room [15.5 min with echo vs 42.4 min without].(2) It can also provide an accurate estimation of ejection fraction compared to “official” echocardiograms (3) and help diagnose pulmonary embolisms at the bedside.(4)
As we have discussed, cardiac ultrasonography has many indications including the estimation of ejection fraction, diagnosis of acute heart failure, detection of a pericardial effusion, and right heart strain in PE…etc… However, none of these applications can be done without understanding the basics of positioning. Practice the techniques described above and stay tuned for future posts on how to detect pathology
Resources:
- Mandavia DP1, Hoffner RJ, Mahaney K, Henderson SO. Bedside echocardiography by emergency physicians. Ann Emerg Med. 2001 Oct;38(4):377-82.
4. Dresden, Scott et al. Right Ventricular Dilatation on Bedside Echocardiography Performed by Emergency Physicians Aids in the Diagnosis of Pulmonary Embolism. Annals of Emergency Medicine , Jan 2014; Volume 63 , Issue 1 , 16 – 24
MEDIA:
gfycat.com/WildTightCaribou
i.ytimg.com/vi/GroiW_kjTKk/hqdefault.jpg
https://upload.wikimedia.org/wikipedia/commons/d/d3/Heart_normal_lpla_echo_view.svg
static1.squarespace.com/static/587a643a6a4963fff6c7b669/58966f5646c3c4ce3435648c/58966f5646c3c4ce3435648b/1485223793130/gif+%2818%29.gif
https://www.researchgate.net/profile/David_Oxborough/publication/222187518/figure/fig6/AS:305049843585029@1449740958356/Figure-6-Parasternal-short-axis-at-the-level-of-the-aortic-and-pulmonary-valves.png
https://www.researchgate.net/profile/David_Oxborough/publication/222187518/figure/fig7/AS:305049843585030@1449740958401/Figure-7-Parasternal-short-axis-at-the-level-of-the-mitral-valve.png
clinicalgate.com/wp-content/uploads/2015/02/B9780323055277500093_gr6.jpg
i.pinimg.com/originals/b0/0c/97/b00c9722e8a52bae4ed14e73b0ff1125.jpg
https://www.researchgate.net/profile/Simon_Dubrey/publication/41172925/figure/fig5/AS:277086464954373@1443073969352/Fig-5-Apical-4-chamber-view-of-a-2-dimensional-echocardiogram-in-a-patient-with-advanced.png
https://web.stanford.edu/group/ccm_echocardio/wikiupload/thumb/1/1b/Apical4.JPG/480px-Apical4.JPG
www.echopedia.org/images/thumb/2/25/Heart_apical_4_chamber.svg/442px-Heart_apical_4_chamber.svg.png
https://web.stanford.edu/group/ccm_echocardio/wikiupload/thumb/0/0f/Schema_apical_4_chamber.jpg/200px-Schema_apical_4_chamber.jpg
www.medison.ru/ultrasound/img/a359.gif
mmartinez
Latest posts by mmartinez (see all)
- Simulation Journal Club: In-Situ Simulation - February 17, 2019
- POCUS: How to Diagnose Appendicitis Using Ultrasound - August 2, 2018
- Luxatio Erecta: Ultrasonography and Reduction - January 15, 2018



0 Comments